Screening vs Assessment. Does it Matter?
FREE step-by-step demonstration

If we don’t know our patients, we can’t give them exactly what they need. As rehab professionals, we all understand the importance of a good evaluation. It guides us and directs what we do with our modalities, manual therapy and exercise programs. There is little doubt that a good evaluation is imperative for positive patient outcomes.
The evaluation process is essential for discovering unknown, underlying issues. There are basically 4 levels of dysfunction that we need to be aware of:
Some would say that the difference between a screen and an assessment is just a matter of semantics. But, there is actually an important distinction between the two. A screen is an evaluation that looks at larger movement patterns to decide if someone is suitable for a particular activity or task. A screen is typically performed in the absence of pain and looks for big, gross abnormalities with the way people move and feel.
An assessment is much more detailed and looks at why someone can’t perform a task. It is usually performed in the presence of pain and typically involves clinical special tests. It is much more diagnostic in nature than a screen and utilizes specific clinical decision-making skills.
You may be asking yourself, if assessments are more detailed and specific, why wouldn’t I just do an assessment on everyone? While that would be great, it just isn’t realistic, nor is it necessary. It would take a long time to assess every single body part of every patient for everything, just hoping to find a few things wrong. Taking that kind of energy and time is excessive and wouldn’t be well tolerated by a lot of our patients.
There are a lot of strategies and philosophies regarding movement screening, but the overall goal is to be able to take a handful of foundational movements and observe people as they navigate their environment. At the end of the day, all movement can be used as a screen as long as you watch people in all 3 planes of movement. But, it is suggested that you look at the following basic patterns that human beings combine to create virtually all of our daily activities:
Both assessments and screens fall within the evaluation process and both of them definitely have their place. Oftentimes screens can be dismissed as not specific enough or cumbersome, so they don’t get performed. That is unfortunate because they have a very specific role in the rehab process and should be utilized on a regular basis with the majority of patients.
Discovery Process
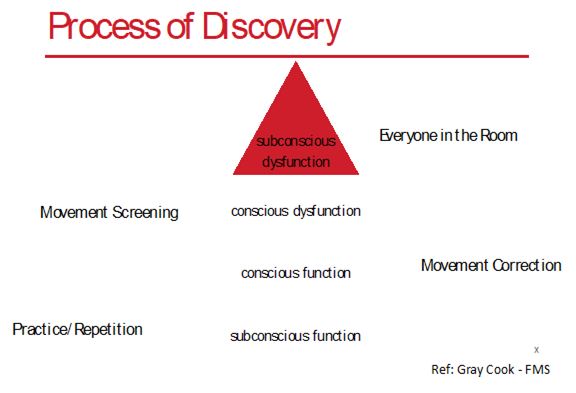
The evaluation process is essential for discovering unknown, underlying issues. There are basically 4 levels of dysfunction that we need to be aware of:
- Subconscious Function: These are things that we perform efficiently and effectively without having to think about it.
- Conscious Function: These are the movements that we perform well when we consciously work at it.
- Conscious Dysfunction: These are the items that are dysfunctional and we are aware of them. They can be troublesome, but because people realize that they are dysfunctional, they typically adapt their movements or surroundings to work around them.
- Subconscious Dysfunction: These are the things that people don’t do well and don’t realize that they don’t do them well. These are the most dangerous of the 4 levels and everyone, on some level, has some amount of subconscious dysfunction.
Screen vs Assessment
Some would say that the difference between a screen and an assessment is just a matter of semantics. But, there is actually an important distinction between the two. A screen is an evaluation that looks at larger movement patterns to decide if someone is suitable for a particular activity or task. A screen is typically performed in the absence of pain and looks for big, gross abnormalities with the way people move and feel.
An assessment is much more detailed and looks at why someone can’t perform a task. It is usually performed in the presence of pain and typically involves clinical special tests. It is much more diagnostic in nature than a screen and utilizes specific clinical decision-making skills.
You may be asking yourself, if assessments are more detailed and specific, why wouldn’t I just do an assessment on everyone? While that would be great, it just isn’t realistic, nor is it necessary. It would take a long time to assess every single body part of every patient for everything, just hoping to find a few things wrong. Taking that kind of energy and time is excessive and wouldn’t be well tolerated by a lot of our patients.
Why screen movement in a rehab setting?
- Guide Your Assessment: It makes a lot of sense to fully assess the area of the body that is the chief complaint. But, we also need to look throughout the body during our evaluation to identify dysfunction in seemingly unrelated areas that contribute to the chief complaint. Whether we use a fascial system, joint-by-joint approach or some other means to look at regional interdependence, it is imperative that we look at a global methodology to movement, regardless of the reason for their visit. By performing an overall screen in addition to the local assessment, we can identify areas that need to be further evaluated. As an example, if someone comes in for shoulder pain, their hip or knee dysfunction may be contributing to their shoulder issue. A quick screen of those areas to look for big dysfunction will indicate whether or not you need to spend the time or energy assessing them.
- Return to Activity: It can be challenging to know exactly when someone is really ready to return to their sport or activity. Many people use simple measurements like strength testing or girth measurements, but those don’t always translate well into the real world. By performing a quick and efficient total body screen, you can rest assured that you have covered all of your movement bases prior to releasing them.
- Injury Screen: As clinicians, we are always looking for new ways to serve our patients and communities. Performing movement screens to otherwise healthy individuals will help to identify a person’s subconscious dysfunction and can be a great way to identify injury risk and provide corrective strategies based on what is identified.
What Should Be Included in a Screen?
There are a lot of strategies and philosophies regarding movement screening, but the overall goal is to be able to take a handful of foundational movements and observe people as they navigate their environment. At the end of the day, all movement can be used as a screen as long as you watch people in all 3 planes of movement. But, it is suggested that you look at the following basic patterns that human beings combine to create virtually all of our daily activities:
- Squat
- Lunge
- Press
- Pull
- Plank
- Rotate
Conclusion
Both assessments and screens fall within the evaluation process and both of them definitely have their place. Oftentimes screens can be dismissed as not specific enough or cumbersome, so they don’t get performed. That is unfortunate because they have a very specific role in the rehab process and should be utilized on a regular basis with the majority of patients.
Do you want to revolutionize your approach to movement?

The key to improving movement quality starts with a high-quality screening tool. If you don’t understand a person’s dysfunction, you will never be able to give them appropriate interventions.
But, screening is just the beginning. Bringing 20 years of movement analysis experience to the program, Mitch Hauschildt, will provide insight for how to screen and enhance movement quality.
This step-by-step process will result in improved clinical outcomes and increased performance in your client population.
You’ll learn exactly why, how, and when to screen your clients and patients and how to correct their faulty movement patterns.
Identify and correct the core issue faster – watch Mitch Hauschildt for Screen, Steer, Move!
But, screening is just the beginning. Bringing 20 years of movement analysis experience to the program, Mitch Hauschildt, will provide insight for how to screen and enhance movement quality.
This step-by-step process will result in improved clinical outcomes and increased performance in your client population.
You’ll learn exactly why, how, and when to screen your clients and patients and how to correct their faulty movement patterns.
Identify and correct the core issue faster – watch Mitch Hauschildt for Screen, Steer, Move!
Meet the Expert:
Mitch Hauschildt, MA, ATC, CSCS, has 20 years of experience as an athletic trainer and certified strength and conditioning Specialist. Mr. Hauschildt obtained both his bachelor’s and master’s degrees from the University of South Dakota. He serves as the prevention, rehab, and physical performance coordinator at Missouri State University, and has also served as the strength and conditioning coach for both men’s and women’s basketball and volleyball.
Mr. Hauschildt is founder and president of Maximum Training Solutions, LLC, and has worked with thousands of athletes throughout his career, including clients who have won World Series rings, played in the NFL, NBA, MLS, and competed in the Olympics. He is a noted speaker on both a regional and national level and has been published multiple times in professional journals and coaching websites.
Learn more about their educational products, including her upcoming live seminars, by clicking here.
Mr. Hauschildt is founder and president of Maximum Training Solutions, LLC, and has worked with thousands of athletes throughout his career, including clients who have won World Series rings, played in the NFL, NBA, MLS, and competed in the Olympics. He is a noted speaker on both a regional and national level and has been published multiple times in professional journals and coaching websites.
Learn more about their educational products, including her upcoming live seminars, by clicking here.
Topic: Movement
Tags: Advice | Body | Enhance Movement | Screening Tool | Strategy | Success | Therapy Tools | Tools



